Welcome to our comprehensive guide on Wells Syndrome in dogs. As pet owners, we must be aware of various health conditions that can affect our furry friends.
Wells Syndrome, also known as Eosinophilic Granulomatosis, is a rare but significant condition that requires attention in veterinary medicine.
This article will delve into the causes, symptoms, and treatment options for Wells Syndrome in dogs.
Whether you’re a concerned pet owner or a veterinary professional seeking information, this article aims to clearly understand this condition.
Wells Syndrome is a dermatological disorder characterized by eosinophils, a type of white blood cell, causing inflammation and granuloma formation.
While this condition is relatively rare in dogs, understanding its nature and implications can aid in early detection and appropriate treatment.
By exploring the causes and triggers, clinical signs, and diagnostic procedures, we can equip ourselves with the knowledge to identify Wells Syndrome in our beloved pets.
The primary goal of this article is to shed light on Wells Syndrome in dogs and its impact on their health and well-being.
Additionally, we aim to provide valuable insights into the available treatment options, including veterinary care, medications, and lifestyle modifications.
By the end of this article, you will have a comprehensive understanding of Wells Syndrome, allowing you to take proactive measures in managing and supporting your dog’s health.
So, let’s embark on this informative journey together and delve into Wells Syndrome in dogs.
By empowering ourselves with knowledge, we can ensure the best care for our four-legged companions and enhance their quality of life.
What is Wells Syndrome in Dogs?
A. Definition and Background
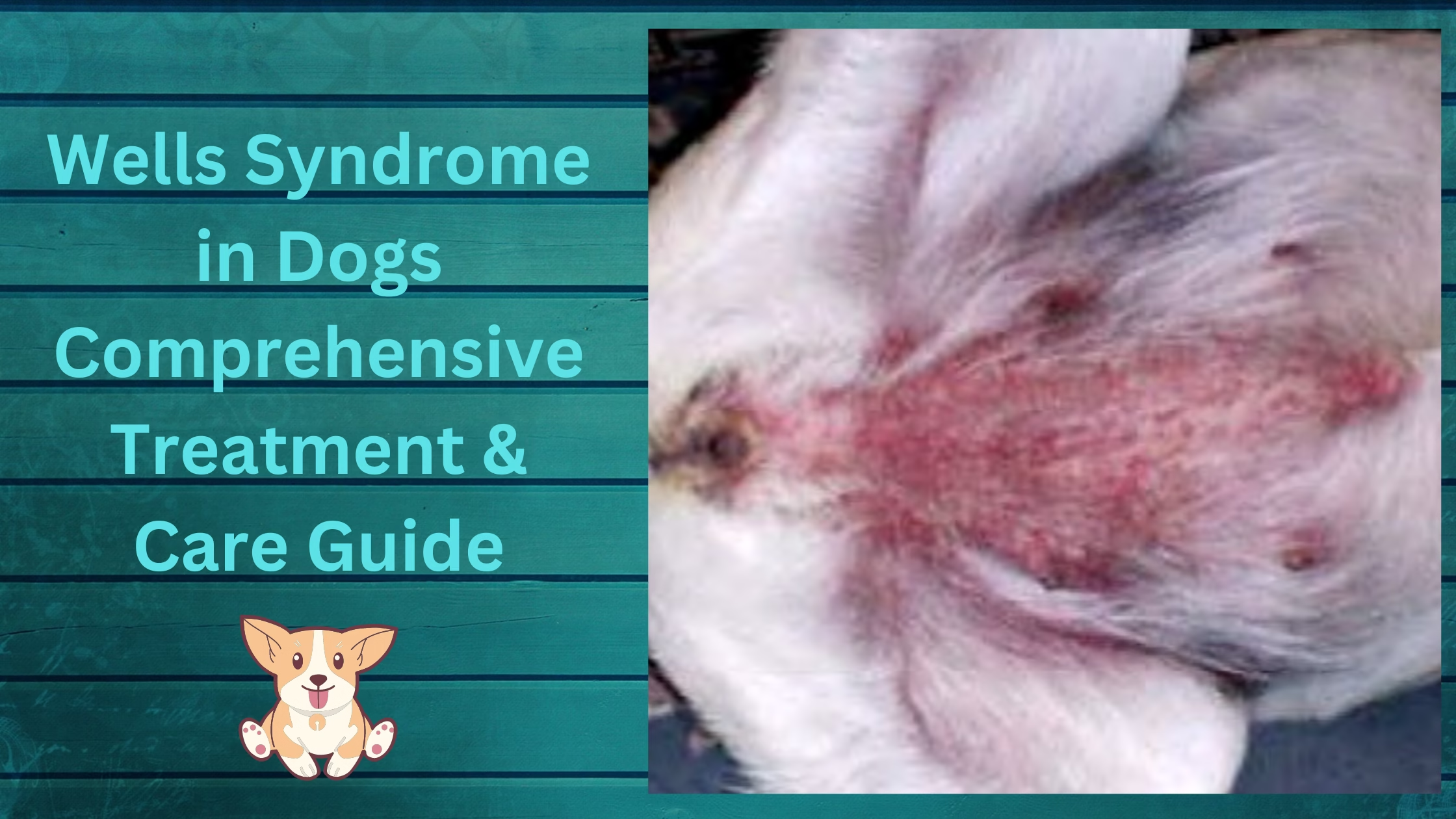
Imagine your dog developing peculiar skin lesions or nodules accompanied by persistent itching.
This could be a sign of Wells Syndrome also known as Eosinophilic Granulomatosis or eosinophilic cellulitis.
Wells Syndrome is a dermatological condition characterized by eosinophils, a type of white blood cell, causing inflammation and the formation of granulomas (small masses of tissue).
It is an uncommon condition in dogs, but its impact on their health should not be overlooked.
Interestingly, Wells Syndrome in dogs shares similarities with its human counterpart. Wells Syndrome is a recognized condition that mainly affects the skin in humans.
It is relatively rare in dogs, making it a topic of interest in veterinary medicine.
Although the exact cause of Wells Syndrome remains unclear, researchers believe it may have immune-mediated components and can be triggered by various factors.
B. Causes and Triggers
The causes and triggers of Wells Syndrome in dogs can vary from case to case. Here are some potential factors that could contribute to the development of this condition:
1. Allergies: Allergens, such as certain foods, environmental substances (pollen, dust mites), or contact irritants, may trigger an allergic response in susceptible dogs.
This hypersensitivity can lead to the development of Wells Syndrome.
2. Infections: In some cases, infections caused by bacteria, parasites, or fungi may play a role in triggering Wells Syndrome.
The immune system response to these infections can result in the characteristic eosinophilic inflammation in affected dogs.
3. Immune System Dysfunction: Disorders that affect the immune system, such as autoimmune conditions, can potentially contribute to the development of Wells Syndrome.
The immune system mistakenly targets healthy tissues in these cases, leading to inflammation and granuloma formation.
It’s important to note that while these factors may contribute to the development of Wells Syndrome, the precise mechanism and triggers can vary between individual dogs.
Identifying the underlying cause of Wells Syndrome is crucial for effective treatment and management.
Understanding the potential causes and triggers of Wells Syndrome provides valuable insight into the condition.
By recognizing the role of allergies, infections, and immune system dysfunction, we can work with veterinary professionals to develop appropriate treatment strategies.
In the following sections, we will explore the symptoms, diagnosis, and treatment options available for Wells Syndrome in dogs, ensuring you are well-equipped to support your furry companion’s health.
Also Read : The American Bulldog Great Pyrenees Mix: A Perfect Blend.
Symptoms and Diagnosis of Wells Syndrome in Dogs
A. Clinical Signs and Presentation
When it comes to Wells Syndrome in dogs, recognizing the symptoms is crucial for timely intervention. Here are some common signs that may indicate the presence of Wells Syndrome in your furry friend:
1. Skin Lesions: Dogs with Wells Syndrome often develop distinct skin lesions or nodules. These can appear as raised, firm, and reddened areas on the skin.
The lesions may vary in size and can be present on any body part.
2. Itching and Scratching: Intense itching is a hallmark of Wells Syndrome. Dogs may frequently scratch, bite, or lick the affected areas to alleviate discomfort.
This can lead to further irritation and potential secondary skin infections.
3. Hair Loss: Dogs with Wells Syndrome may experience localized or generalized hair loss in the affected areas due to constant scratching and inflammation.
This can contribute to the appearance of bald patches or thinning fur.
4. Swelling and Inflammation: In some cases, the affected areas may exhibit swelling or inflammation. This can make the skin appear puffy or thickened, adding to the discomfort experienced by the dog.
It’s important to note that these symptoms vary in severity from case to case.
Suppose you notice any of these signs in your dog. In that case, seeking veterinary attention for a proper diagnosis is recommended.
B. Diagnostic Procedures
Veterinarians may employ several diagnostic procedures to accurately diagnose Wells Syndrome in dogs.
These steps help rule out other potential causes and confirm the presence of Wells Syndrome. Here are some common diagnostic steps:
1. Physical Examination: A thorough physical examination allows the veterinarian to assess the skin lesions, observe the dog’s behavior, and gather essential information for further evaluation.
2. Skin Biopsy: A skin biopsy involves taking a small sample of the affected skin for microscopic examination.
This procedure helps identify the characteristic eosinophilic inflammation and granuloma formation associated with Wells Syndrome.
3. Blood Work: Blood tests may be conducted to evaluate the dog’s overall health, check for any underlying infections, and assess the eosinophil levels in the bloodstream.
Elevated eosinophil counts can provide supporting evidence for the diagnosis of Wells Syndrome.
4. Ruling Out Other Conditions: Since some symptoms of Wells Syndrome overlap with other skin conditions, it is important to rule out alternative diagnoses.
This may involve additional tests such as fungal cultures, skin scrapings, or allergy testing.
By conducting a comprehensive evaluation and ruling out other potential causes, veterinarians can confirm the presence of Wells Syndrome in dogs.
This sets the stage for developing an appropriate treatment plan tailored to your dog’s needs.
The next section will explore the available treatment options and management strategies for Wells Syndrome in dogs, ensuring your furry companion receives the best possible care.
How do you treat Wells syndrome in dogs?

A. Veterinary Care
When treating Wells Syndrome in dogs, seeking veterinary care is paramount. A veterinarian will assess the severity of the condition and recommend appropriate treatment options.
Here are some common treatment approaches for Wells Syndrome:
1. Medications: Medications are key in managing Wells Syndrome in dogs. The primary goal is to reduce inflammation and alleviate itching.
Corticosteroids, such as prednisolone or prednisone, may be prescribed to suppress the immune response and control symptoms.
If previously administered, discontinuing the use of metronidazole may also be recommended as it could potentially be associated with Well’s-like syndrome in dogs.
2. Antihistamines: Besides corticosteroids, antihistamines may help relieve itching and minimize allergic reactions associated with Wells Syndrome.
3. Immunosuppressive Drugs: In more severe or refractory cases, veterinarians may consider immunosuppressive drugs.
These medications help modulate the immune system’s response and effectively control the inflammation associated with Wells Syndrome.
However, their usage requires careful monitoring and veterinary supervision due to potential side effects.
4. Antibiotics: If secondary infections are present due to self-inflicted wounds or compromised skin, antibiotics may be prescribed to treat the bacterial infection and prevent further complications.
B. Lifestyle Modifications
In addition to medication, certain lifestyle modifications can greatly contribute to managing Wells Syndrome in dogs. Here are some recommendations to consider:
1. Avoiding Triggers: Identifying and avoiding potential triggers can help minimize flare-ups.
Allergy testing may be beneficial in identifying specific allergens that could contribute to the condition.
Environmental allergens, certain foods, or contact irritants should be identified and eliminated.
2. Good Skin Hygiene: Good skin hygiene is crucial for dogs with Wells Syndrome.
Regular bathing with a gentle, hypoallergenic shampoo can help soothe the skin, remove allergens, and prevent secondary infections.
However, it’s important not to over-bathe, as excessive bathing can dry and worsen the skin.
3. Nutritional Considerations: A healthy and balanced diet can support your dog’s immune health.
Consult with your veterinarian to determine if any dietary modifications or supplements can be beneficial for managing Wells Syndrome.
4. Environmental Control: Minimizing exposure to potential allergens or irritants in the dog’s environment can help reduce the frequency and severity of flare-ups.
This may involve keeping the living area clean, using allergen-proof bedding, and avoiding known triggers.
By working closely with a veterinarian and implementing these treatment options and lifestyle modifications, you can effectively manage Wells Syndrome in your dog.
Regular follow-up visits with the veterinarian are crucial to monitor progress, make necessary adjustments to the treatment plan, and ensure your furry companion’s well-being.
In the next section, we will discuss the prognosis of Wells Syndrome in dogs and the importance of ongoing care and monitoring.
Prognosis and Follow-up Care for Dogs with Wells Syndrome
A. Outlook for Dogs with Wells Syndrome
Regarding the prognosis of dogs with Wells Syndrome, the outlook can vary depending on several factors.
While Wells Syndrome can be a chronic condition, early detection, and appropriate management can greatly improve the quality of life for affected dogs. Here are some important points to consider:
1. Potential Long-Term Effects: With proper treatment and management, many dogs with Wells Syndrome can experience significant improvement in their symptoms.
However, it’s important to note that some dogs may experience long-term effects, such as scarring or pigmentation changes in the affected areas.
2. Remission and Recurrence: In some cases, dogs may enter a period of remission where symptoms subside or disappear completely.
However, it’s crucial to remain vigilant. Wells Syndrome can sometimes recur, especially if triggers are not properly identified and managed.
B. Monitoring and Follow-up
Regular monitoring and follow-up care are essential to ensure the best possible outcome for dogs with Wells Syndrome. Here’s why it’s important:
1. Veterinary Check-ups: Regular visits to the veterinarian allow for ongoing monitoring of the dog’s progress.
The veterinarian will assess the response to treatment, make any necessary adjustments to the medication regimen, and address any concerns or questions you may have.
2. Medication Adjustments: The initial treatment plan may need to be modified based on the dog’s response and any side effects observed.
The veterinarian will closely monitor the dog’s overall health, including blood work, to check for potential medication-related issues.
Medication dosage or frequency adjustments may be necessary to maintain optimal control of the condition.
3. Proactive Management: Staying proactive is key since Wells Syndrome can have flare-ups or potential recurrences.
This includes maintaining good skin hygiene, avoiding triggers, and promptly seeking veterinary attention if any new symptoms or changes occur.
Remember, each dog’s journey with Wells Syndrome is unique. By staying informed, maintaining open communication with your veterinarian, and providing consistent care, you can help your furry companion live a comfortable and fulfilling life.
Also Read : Husky American Bulldog Mix – Unleashing the Energetic Charm
Conclusion
Wells Syndrome in dogs can present unique challenges. Still, dogs can lead happy and healthy lives with proper understanding, treatment, and ongoing care.
You can effectively manage the condition by recognizing the common symptoms, seeking veterinary care, implementing appropriate treatment options, and incorporating lifestyle modifications.
Regular veterinary check-ups and close monitoring are essential to track progress, make any necessary adjustments to the treatment plan, and ensure the best possible outcome for your furry friend.
With your dedication and support, you can provide the care and attention needed to manage Wells Syndrome in your beloved dog. Together, we can prioritize their well-being and quality of life.